Organ donation in the United States is undergoing a major shift: more organs are now being recovered after the heart stops, rather than after brain death. This trend, known as donation after circulatory death (DCD), could expand transplant availability but also raises public confusion and ethical questions.
According to a new study by NYU Langone Health, DCD accounted for 49% of all deceased organ donors in 2025, up sharply from just 2% in 2000. The rise is largely due to advances in technology that preserve organs as the heartbeat winds down, helping overcome previous limitations and allowing lifesaving transplants for patients on the national waiting list—currently over 100,000 people.
“Donation after circulatory death is complex, and we need to make sure we are doing it well,” said Dr. Babak Orandi, NYU transplant surgeon and co-author of the study. “Stopping or severely restricting it would have serious consequences for patients.”
How Donation After Circulatory Death Works
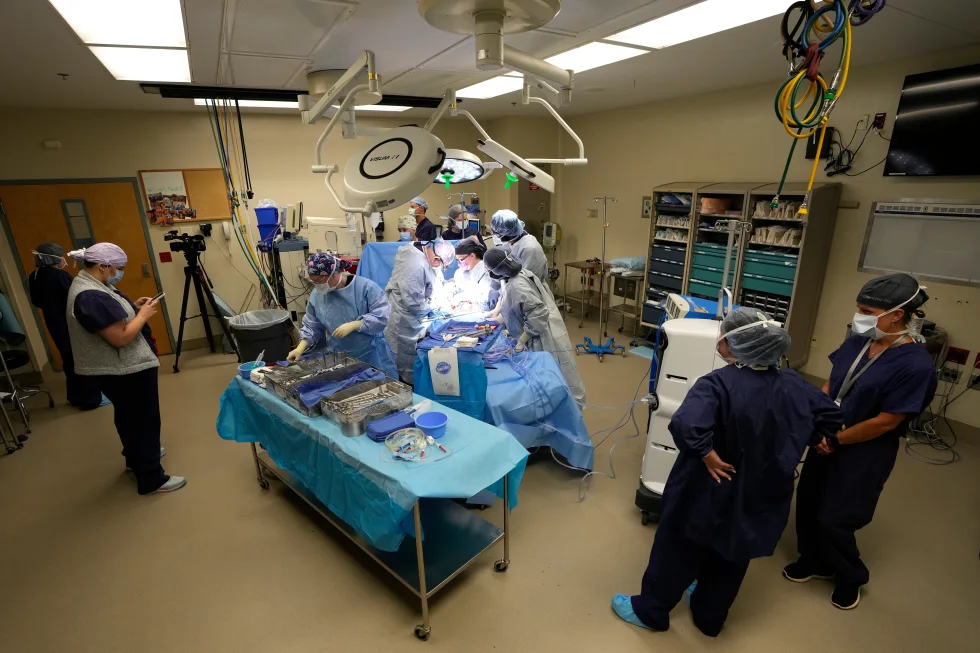
DCD occurs when a patient has a nonsurvivable injury but has not experienced full brain death. With family consent, life support is withdrawn, and the patient’s heart gradually stops. After a mandatory five-minute waiting period to confirm death, organ retrieval can begin.
Unlike brain-death donations, where organs are maintained on ventilators until retrieval, DCD requires special techniques such as normothermic regional perfusion, which temporarily restores blood flow to organs in the chest or abdomen to prevent deterioration. This method has expanded the use of organs from older or less healthy donors, though it has prompted ethical discussions.
By law, transplant teams cannot participate in the decision to withdraw life support, and retrieval only occurs after death is formally declared. If the patient’s heart does not stop within roughly two hours, organs cannot be used.
Regional Differences and Hospital Factors
The study found wide variation in DCD adoption across the country. Some organ procurement organizations (OPOs) report more than half of their donors via DCD, while others have as little as 11%. Hospital size, resources, familiarity with DCD procedures, and availability of preservation technology influence participation.
“Donation after circulatory death requires buy-in from the community, including local hospitals, to make this happen,” Orandi said. “A few problematic cases can undermine public trust in the system.”
New Policies and Safeguards
To address concerns and increase public confidence, the Health Resources and Services Administration is proposing new national guidelines. These include:
- Allowing staff to pause donor preparations if there’s uncertainty about patient eligibility.
- Ensuring hospitals perform proper neurological exams before DCD.
- Educating families about the process of withdrawal and organ recovery.
The Association of Organ Procurement Organizations recommends that life support withdrawal occur in the intensive care unit rather than the operating room to reduce confusion about the timing of death relative to organ retrieval.
With these changes, experts hope to increase the number of lifesaving transplants while maintaining ethical standards and public trust in the donation system.